Your dog has been drinking more water lately. You’ve noticed it — the bowl emptying faster, the extra trips outside, maybe an accident or two in the house from a dog who hasn’t had one in years. You almost brush it off. Dogs have off days. It’s probably nothing.
It might be nothing. But if that pattern holds for more than a few days, it is worth taking seriously. Because one of the most common reasons a dog starts drinking and urinating excessively is kidney disease — and the earlier you catch it, the more time and quality of life you can give your dog.
Kidney disease in dogs is one of those conditions that hides in plain sight. The early signs are quiet, gradual, and easy to explain away. By the time most owners recognize something is genuinely wrong, the disease has often been progressing for months. That is not a failure of love. It is the nature of how kidney disease works. But understanding what to look for, why the kidneys fail, and what you can actually do about it changes the outcome significantly.
This is everything you need to know.
Table of Contents
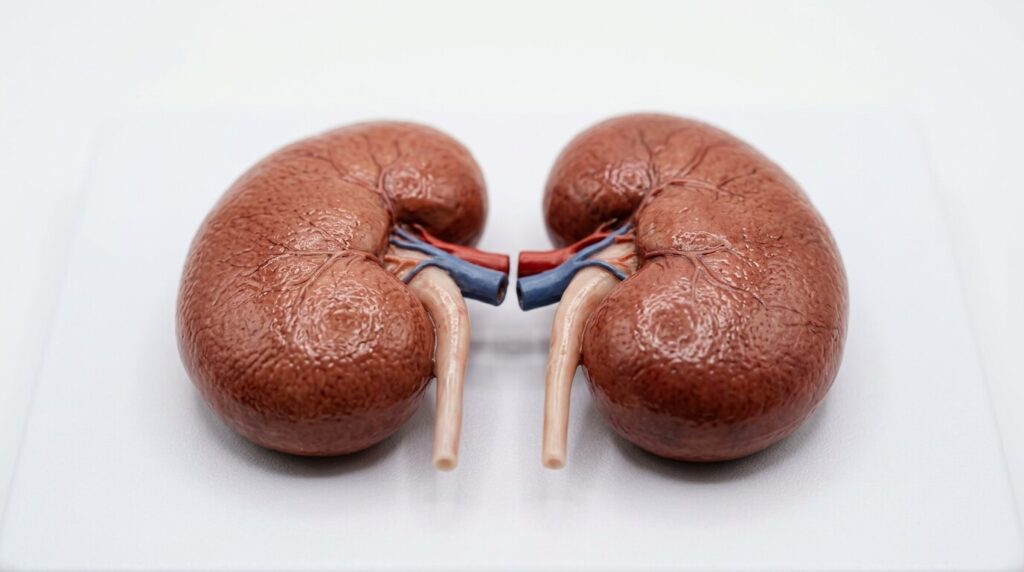
What the Kidneys Actually Do
Before you can understand what goes wrong, it helps to understand what the kidneys are doing right every single day.
Your dog’s kidneys are two small organs working around the clock to filter waste products out of the blood, regulate fluid and electrolyte balance, control blood pressure, and produce hormones that support red blood cell production. They are, in short, doing an enormous amount of work quietly in the background — and they are remarkably resilient. A dog’s kidneys can continue functioning well even when up to two-thirds of their capacity has been lost.
That resilience is both a blessing and a challenge. It means your dog can live comfortably with significant kidney damage. It also means that by the time symptoms become obvious, the disease is already well established.

The Early Signs of Kidney Disease in Dogs
The earliest signs of kidney disease are easy to miss precisely because they look like so many other things. Here is what to watch for.
- Increased thirst and urination are almost always the first signs an attentive owner notices. You find yourself refilling the water bowl more often. Your dog is asking to go outside every couple of hours instead of his usual four times a day. He might start having accidents indoors — not from laziness or behavioral issues, but because his kidneys are no longer concentrating urine efficiently, forcing his body to produce more of it. The urine itself may be very pale, almost colorless, or have an unusually strong odor. In some cases you might notice a darker tinge or even trace amounts of blood.
- Changes in appetite and weight often follow. Your dog — the one who used to clean his bowl in thirty seconds flat — starts walking up to his food, pausing, and walking away. He might drool slightly near the bowl, which is a sign of nausea. Over weeks, you start to notice he looks thinner, even if his eating seems mostly normal.
- Bad breath with an unusual quality is one of the more telling signs that many owners overlook. When the kidneys stop filtering waste products effectively, those toxins accumulate in the bloodstream and eventually make their way into the breath. The result is a smell that is distinct from ordinary dog breath — often described as ammonia-like or chemical. If your dog’s breath has shifted in a way you can’t quite put your finger on, it is worth mentioning to your vet.
- Pale gums are another sign worth knowing. Healthy dog gums should be a moist, bubblegum pink. In dogs with advancing kidney disease, anemia can develop as the kidneys lose their ability to stimulate red blood cell production — and pale, washed-out gums are one of the visible signs of that anemia.
- Mouth sores or ulcers can develop in more advanced cases, caused by the buildup of uremic toxins in the body. These are uncomfortable and can make eating even more difficult for an already nauseous dog.
- Lethargy and rear-end weakness round out the picture. Your dog may seem less interested in walks, slower to get up, or generally less engaged with the things that usually excite him. Some dogs show a subtle weakness in their hind legs that owners initially mistake for arthritis or general aging.
It is worth saying clearly: none of these symptoms on their own confirms kidney disease. Increased thirst can indicate diabetes. Pale gums can signal other forms of anemia. Weight loss has dozens of possible causes. What should prompt a vet visit is when two or more of these signs appear together — especially in a dog over seven years old.

What Causes Kidney Disease in Dogs?
Kidney disease is not one single condition. It is an umbrella term covering several different situations, each with its own cause and trajectory.
Age-Related Decline:
The most common form of kidney disease in dogs is chronic kidney disease (CKD) in senior dogs — and sometimes the honest answer is simply that the tissues are wearing out. Just as human kidneys lose efficiency with age, a dog’s kidneys gradually decline over time. This is not a failure of care or nutrition. It is biology. What matters is how early you catch it and how well you manage it.
Congenital and Genetic Defects:
Some dogs are born with kidney problems or inherit conditions that affect kidney development. Renal dysplasia — where the kidney tissue doesn’t develop normally — can cause puppies to show signs of kidney failure very early in life. These puppies often drink and urinate excessively, struggle to gain weight, and fall noticeably behind their littermates in development. They are frequently described as “failure to thrive.”
Polycystic kidney disease is another inherited condition, and amyloidosis — a condition where abnormal protein deposits accumulate in the kidneys — is seen with particular frequency in Chinese Shar Peis. Some genetic kidney conditions don’t become clinically apparent until a dog is six or seven years old, which is worth knowing if you have a breed with known kidney vulnerabilities.
Toxin Exposure:
This is where acute kidney failure enters the picture — and it is a different beast entirely from the gradual decline of chronic disease. Certain toxins cause rapid, severe kidney damage that requires emergency treatment.
The list of culprits includes acetaminophen (Tylenol), grapes and raisins (even small amounts), ethylene glycol (antifreeze), and certain antibiotics and medications. If your dog has been exposed to any of these and is showing signs of vomiting, collapse, intense thirst, or seizures — do not wait. Get to a veterinary clinic immediately. With rapid treatment, some dogs recover completely. Without it, acute toxic kidney failure can be fatal within hours.
Infections and Illness:
Bacterial and viral infections that reach the kidneys can cause lasting damage. Lyme nephritis — a complication of Lyme disease — has become increasingly common as tick-borne illness spreads to new regions. Veterinarians now routinely monitor dogs with known Lyme disease exposure for early signs of kidney involvement, typically by checking for protein spillage in the urine. Any serious systemic infection has the potential to affect kidney function, which is one of the reasons prompt treatment of infections always matters.

How Kidney Disease is Diagnosed
If your vet suspects kidney disease based on the symptoms you describe, they will want a complete blood panel and a urinalysis. These two tests together give a detailed picture of how the kidneys are functioning.
The blood panel will look at levels of creatinine and BUN (blood urea nitrogen) — both of which rise when the kidneys are struggling to clear waste from the blood. It will also assess electrolyte levels, red blood cell count, and overall organ function.
The urinalysis looks at how well the kidneys are concentrating urine, whether protein is spilling through (which it shouldn’t be), and whether there are any signs of infection or blood.
One test worth specifically requesting for dogs over seven is SDMA — symmetric dimethylarginine. This is a biomarker that can detect kidney dysfunction when as little as 25% of kidney function has been compromised, which is significantly earlier than creatinine levels typically rise. Many senior blood panels now include SDMA automatically, but if yours doesn’t, ask for it. Results above 14 micrograms per deciliter suggest early kidney changes that warrant closer monitoring. Catching the disease at this stage — before symptoms are even obvious — is where the biggest difference in outcome is made.
Kidney disease is formally staged using the International Renal Interest Society (IRIS) system, which uses creatinine levels, blood pressure, and urine protein levels to place a dog in one of four stages. The stage determines the treatment approach and gives your vet a framework for monitoring progression over time.

Treating Kidney Disease in Dogs
The first thing to accept — and it is a hard one — is that kidney disease cannot be reversed. Damaged kidney tissue does not regenerate. What treatment does is slow the progression of the disease, manage symptoms, and protect the remaining functional kidney tissue for as long as possible. For many dogs, that means years of genuinely good quality life.
Hydration
Keeping a dog with kidney disease well hydrated is one of the most important things you can do, because the kidneys need adequate fluid to function and to flush waste products from the body. Start with fresh, clean water always available. Switching from dry kibble to wet food makes a meaningful difference — canned foods typically contain over 70% moisture compared to around 10% in dry food. As the disease progresses, many dogs benefit from subcutaneous fluid therapy administered at home — a technique your vet can teach you, and one that many owners become confident with quickly.
Medications:
Depending on the stage of disease, your vet may prescribe phosphate binders to reduce the amount of phosphorus absorbed from food, medications to control blood pressure (which when elevated accelerates kidney damage), and anti-nausea medications to help your dog eat comfortably. Dogs who develop significant anemia may be prescribed darbepoetin, a synthetic hormone that stimulates red blood cell production.
Dialysis and Transplants
Dialysis is rarely used for chronic kidney disease in dogs but can be genuinely life-saving for a dog with acute toxic kidney failure. It is currently only available at a small number of veterinary colleges and specialty centers. Kidney transplants have been performed in dogs but are significantly less successful than in cats, require a compatible living donor (who you are then responsible for adopting), and demand lifelong immunosuppressive medication. For most families, this is not a realistic path — but it is worth knowing the option exists in the most serious cases.

The Kidney Diet: What Your Dog Should and Shouldn’t Be Eating
Diet is not a side note in kidney disease management. It is one of the most powerful tools you have. The right diet can meaningfully slow the progression of the disease and significantly improve your dog’s comfort and energy levels. The wrong diet can accelerate kidney damage. Here is what the science actually says;
Protein: Less Is Not Always More
For years, the standard recommendation for dogs with kidney disease was to put them on a very low protein diet. The thinking made sense — protein metabolism produces waste products that the kidneys have to filter, so less protein should mean less work for the kidneys.
The current understanding is more nuanced. Very low protein diets can cause muscle wasting, reduce palatability (meaning your dog won’t eat), and deprive the body of essential amino acids it genuinely needs. The current recommendation is moderate amounts of high-quality, highly digestible protein — not the lowest protein possible.
What does high quality mean in practice? The protein in eggs is considered 100% digestible. Chicken, beef, and lamb come in at 90 to 95% digestibility. These are the kinds of proteins that deliver what the body needs without generating excessive waste. Poor-quality protein from heavily processed sources does the opposite — it creates metabolic work without the nutritional payoff.

Phosphorus: This One Genuinely Matters
If there is one dietary factor that has the strongest evidence behind it in kidney disease management, it is phosphorus restriction. When the kidneys are damaged, they lose the ability to excrete phosphorus efficiently. Phosphorus accumulates in the blood, triggering the release of parathyroid hormone — and chronically elevated parathyroid hormone actively accelerates kidney deterioration. It becomes a damaging cycle that proper dietary management can interrupt.
Foods high in phosphorus include organ meats, dairy, bones, and to a lesser extent muscle meats. Commercial kidney diets are specifically formulated with this in mind. If you are feeding a home-cooked or raw diet, phosphorus management requires careful attention and ideally guidance from a veterinary nutritionist.
Bone broth, despite its reputation as a health food for dogs, is something to be cautious with in dogs with kidney disease — it can be high in both phosphorus and sodium.
Omega-3 Fatty Acids: One of the Best Things You Can Add
EPA and DHA — the omega-3 fatty acids found in fish oil and marine microalgal oils — have documented anti-inflammatory and kidney-protective effects. Supplementing with a quality fish oil like salmon oil is one of the more straightforward and evidence-supported additions you can make to a kidney disease diet.
One important distinction: omega-6 fatty acids, found in safflower and sunflower oils, appear to be detrimental to kidney health in dogs with CKD. This is worth checking on any commercial food you are considering — look at the fat sources listed in the ingredients.
Antioxidants: Supporting the Body’s Defenses
Free radicals — unstable molecules produced through normal cellular processes — cause oxidative damage to tissues throughout the body, and that damage has been specifically linked to the progression of kidney disease. Vitamins E and C are the antioxidants most commonly supplemented in kidney disease management, helping to neutralize free radicals and reduce the inflammatory load on already-stressed kidney tissue.
Sodium: Keep It Reasonable
Damaged kidneys have a reduced ability to regulate sodium. Excess sodium contributes to elevated blood pressure, which then causes further damage to the delicate filtration structures within the kidneys. Restricting dietary sodium is a precautionary measure that makes genuine sense in this context — not an arbitrary limitation.
Water: More Than You Think
Fresh water should always be available, and more is better. Some dogs with kidney disease benefit from having multiple water bowls placed around the house. Ice cubes made from plain water can encourage drinking in dogs who seem less interested in their bowl. If you add anything to water to make it more appealing — and some owners do — choose options that are low in sodium and phosphorus.

Living Well With Kidney Disease
A diagnosis of kidney disease is not the end of the story for your dog. It is actually a turning point — and how you respond to it determines what comes next.
Dogs caught in the early stages of CKD, properly managed with the right diet, appropriate hydration, regular monitoring, and medications when needed, can live for years with genuinely good quality of life. They play. They eat. They do the things that make them happy. The disease is present, but it is not in control.
What makes the difference, almost every time, is how early the disease is found. Annual blood panels and urinalysis starting at age seven — and specifically including that SDMA test — are not optional extras for a senior dog. They are the tool that gives you the head start you need.
Watch the water bowl. Notice the changes. Trust your instincts when something feels different. Your dog cannot tell you when something is wrong. But if you know what to look for, you will see it.
At For Better For Dogs, we believe that understanding your dog — really understanding them — is the most powerful form of care there is. Have a question about kidney disease or want to share your experience managing it with your own dog? Leave a comment below. We read every single one.
